Introduction
The lamentable position that is often tossed around this site as well as others, including this site’s precursor, is that single payer healthcare will be implemented within the lifetime of the current generation. While the majority of the intended audience may not fall into this demographic, others here will probably experience this for themselves. This series of essays is not necessarily intended to be an advocacy piece. This is intended to provide a snapshot of a healthcare system that is currently in place in the United States today, that embodies everything a single payer system in a ‘civilized’ nation such as those in Western Europe, Canada and elsewhere. Governments tend not to be innovative, and instead will opt for a solution with a historical basis for which an ‘educated’ opinion can be determined. In other words, if and when this happens it will not be a brand new system but one which will be based on prior experience and there is only one American system today that has the capacity, scope and history for which to base a single payer system. The problem of course, is the system in question is only available for an surprisingly small group of Americans and many who may argue against such a system are not likely to have experienced it for themselves. As Sun Tsu once postulated in order to defeat the enemy, one must know the enemy better than they know themselves.
 If advocates of free markets, Federalism and personal responsibility are to define coherent arguments against such a system it is best they first understand what the future may look like. While the practical experience in Western Europe should provide enough ammunition, it is likely these systems will be used as arguments for single payer systems. It should however be noted, the experience in these countries are unlikely to be comparable to the United States, because these governments historically are more enthusiastic(?) in their approach to governance. Not to mention the centralized nature of the population and demographic homogeneity make it easier for these socialized systems to be implemented. An American example is needed–and fortunately is available for interpretation. It is this way freedom advocates will know, and knowing is half the battle.
If advocates of free markets, Federalism and personal responsibility are to define coherent arguments against such a system it is best they first understand what the future may look like. While the practical experience in Western Europe should provide enough ammunition, it is likely these systems will be used as arguments for single payer systems. It should however be noted, the experience in these countries are unlikely to be comparable to the United States, because these governments historically are more enthusiastic(?) in their approach to governance. Not to mention the centralized nature of the population and demographic homogeneity make it easier for these socialized systems to be implemented. An American example is needed–and fortunately is available for interpretation. It is this way freedom advocates will know, and knowing is half the battle.
This is the Veterans Health Administration (VHA). As interpreted by a mid-level GS employee with direct experience at the VISN (regional) and Facility level.
Eligibility
The first thing any health care system will need to determine is the eligibility requirements to utilize the services provided by the system. Without boundaries, there will be no limitations to the extent these services are rendered.
In conceptual terms, eligibility is the first form of control. This is to determine who gets in, and among those, what can be allocated.
First thing first, nearly everyone using VHA services are Veterans but not all are combat veterans. There are Veterans that were given a disability for other reasons, such as injuries during peacetime, asthma or sexual trauma, which unlike its counterpart on college campuses actually did happen to a good extent in the past. There even are some annoying situations where Veterans of some wars are simply viewed as better than others. WWI and the Mexican Border War Veterans for example, assuming there are any living examples, by law are currently allowed unlimited access to all services at any VHA facility (1).  While Eddie Rickenbacker does not need to worry about paying for a colonoscopy, there are others with ailments such as Agent Orange or Gulf War Syndrome that were affiliated with wars that were determined by popular culture to be unpopular from a political standpoint, and were thus swept under the rug.
While Eddie Rickenbacker does not need to worry about paying for a colonoscopy, there are others with ailments such as Agent Orange or Gulf War Syndrome that were affiliated with wars that were determined by popular culture to be unpopular from a political standpoint, and were thus swept under the rug.
For good reason, with his hat tilted the wrong way and his hands conspicuously in his pocket, America’s first ace has the kind of swagger that will drive a Sgt. Major to the brink of insanity. Most can only dream of such awesomeness. Therefore Mr. Rickenbacker should not need to worry about his access to quality healthcare and he is not at all worried–because he is dead.
For everyone else, it is a process that begins at a recruiting station when nobody is old enough, or even cognizant of the future’s possibility. Nobody discusses VHA benefits with a recruiter, because quite frankly even the recruiter does not know because he or she is not to that point in their life either. This process starts at the end of an enlistment or near retirement. Once a retiree drops the paperwork at the personnel office or upon signing the separation paperwork, they are eligible to apply for disability. The math on this is not what most consider to be math to begin with.
 For most sane individuals with the most rudimentary of education, 10+10+20=40, right?
For most sane individuals with the most rudimentary of education, 10+10+20=40, right?
Wrong!
The VA uses a descending efficiency scale (2). What this means, is the government decided that math was too straightforward and made a system of it. Essentially, a service member shows up at the recruiting office at 100% because most of the recruiting process is determining medical qualifications. The military is quite efficient at weeding out those that are not at 100%. It is assumed the service member will incur some type of injury that will negatively affect the rest of his or her life. For instance, asthma as previously mentioned will net the service member a 30% disability. Hearing loss is another 10% resulting in a total of 30% disability. How? Asthma reduced him to 70% of his initial ability. Now that he can only hear in his left ear, reduces that 70% by another 7%, because 10% of seventy is seven.
30+7=37 rounded down to the nearest 10 is 30. Get it?
Most Veterans will fall into the trap where they tell a doctor something hurts, therefore it affects them negatively. This is not how it works. The doctor performing a Compensation & Pension Examination is concerned about how the condition will inhibit your ability to function from a quality of life standpoint. In other words does it keep you from getting a job? Back pain does not prevent one from working the concierge desk at the local Marriott, nor does being wheelchair bound keep one from working at a bank. It will keep them from working a high paying job on a oil rig, railroad or construction site. The post industrial job market, the Montgomery (later Post 9/11) GI Bill and the Americans with Disability Act do provide some relief for those alternatively abled. In order to help the Veteran handle his pain physically, the VHA has a well negotiated prescription drug formulary. It is designed to control the cost of medication, and thus facilitate a solution for pain relief.
Now this service connection will net the service member (now considered a Veteran) a disability payment that will need to be paid monthly as long as the Veteran lives. Per the numbers ran by the associated press the last time Veterans were used as a political hot potato during the Sen. Ted Cruz led government shutdown of 2013, this is around $5 billion–monthly (3).
Once a Veteran has a service connected disability (SC), they are deemed eligible for VHA healthcare–even if that disability is 0%.
Why is eligibilty so important? The system needs to know how many it must serve. The health insurance industry also has a concept tossed around from time to time known as ‘moral hazard.’ What this means is the more an individual is insulated from the costs of the services being paid for, the more likely they will use the service. This needs to be accounted for in order to control their costs. In other words, people will not care if it is not their money at stake. This is a concept familiar to many free-market aficionados. There is also the small issue of Veterans and non-Veterans alike in abusing the system to enrich themselves financially(4) . Most of these are, hopefully, outliers but abuses to the system also lead to inefficiencies caused by programs within the system designed to ensure the program’s solvency, which leads to Veteran’s waiting a long time for their eligibility paperwork to be processed.
This SC rating translates to how a VA Medical Center (VAMC) is funded.
Funding
If only it were simple to explain how a VAMC is funded: Congress does not write into a budget that VAMC Tom, Dick and Harry shall receive $X. The system is designed so that the Veteran population can be in flux and the allocation can reflect how ‘sick’ that particular population is and how often it is used. It is based on disability, age and other factors, like if a Veteran received a Medal of Honor, a Purple Heart, was a Prisoner of War, and the like. Sgt. Dakota Meyer has two out of the three mentioned, and that ain’t bad. Then again, so does Sen.
John McCain.
 The bottom line is, the more service connected the Veteran is and the greater resources it would theoretically take to treat the Veteran individually, the more money the VAMC receives from Washington. This is not just for the big things like, a prosthetic or a cochlear implant that are SC, this also works for little things like flu shots and almost everything else Veterans use that is not SC. The dirty secret is, most services Veterans use at a VAMC are not SC, even if he or she is 100%. This funding system is called Veteran’s Equitable Resource Allocation (VERA).
The bottom line is, the more service connected the Veteran is and the greater resources it would theoretically take to treat the Veteran individually, the more money the VAMC receives from Washington. This is not just for the big things like, a prosthetic or a cochlear implant that are SC, this also works for little things like flu shots and almost everything else Veterans use that is not SC. The dirty secret is, most services Veterans use at a VAMC are not SC, even if he or she is 100%. This funding system is called Veteran’s Equitable Resource Allocation (VERA).
The cited report from the Rand Corporation is predictably thorough in its methodology, analysis and description of the VERA system. The highest VERA category is about $70,000/year. This is designed to put a higher value on Veterans that need the care versus the ones that may not, and cover the cost difference of the former with the latter. A Las Vegas oddsmaker works in a similar fashion. It should be pointed out, Rand’s overall assessment of the system and its efficiency is highly dependent upon the Veterans that are also eligible for Medicare(5) . In short, the overall cost of care for Veterans is largely uncertain for any that are over 65. The reason being, VHA is unable to bill Medicare for services, much like one does not bill their spouse for services performed around the house. Ultimately, the proceeds from such a transaction are coming from and going to the same budget. Since many Veterans are part of this demographic or soon will be, it is likely the cost to providing Veterans health care is going to be skewed by this factor. What makes this more difficult to quantify, is HIPAA and that Medicare providers are under no obligation to provide VHA with medical records for services that are not provided under VHA auspices.
In fact, this factor was cited by Longman as an argument to save costs on Medicare. It is estimated VHA has a lower overall cost of care due to the VHA ownership in facilities and control of the services in terms of medical necessity, by about ⅔ the cost of Medicare. In a CBO report reviewing costs from 2007-2015, it was estimated that putting Veterans qualifying for Medicare back on VHA would save $29.5 Billion over the time period, with $4.8 Billion saved from Medicaid(1) .
Third party revenue can also be captured by VHA. This is allowed under the Balanced Budget Act of 1997(6) where the VAMC can code and bill a private insurance company the same way as any health system. The difference being they are only able to bill if the Veteran has other health insurance and are financially capable of paying a $15 or $50 copay. Under the PPACA, the IRS will automatically notify VHA if the Veteran has other health insurance. This accounts for 10-20% of a VAMC budget.
There are other ways to fund specific programs such as prescription drugs, durable medical equipment, real estate, furniture and NonVA Care. These however, are largely allocated to VAMC a with a specific purpose. There is some discretion on how VERA funds can be allocated between facilities, but this is for the most part, a reaction to the present circumstances and typically planned within a fiscal a year. This is how a VAMC can install millions of dollars worth of solar panels in the parking lot but somehow fall short of their budgetary obligations with few repercussions.
Ruminations on Eligibility and Funding
From experience with eligibility, a moral case can be made on determining who is eligible. Some questions that may be raised include:
– Does a minority, or anyone from a supposedly aggrieved demographic deserve more or less than a white male between the ages of 18-55?
– Does an individual with late stage cancer receive a higher allocation than a single mother with 4 kids?
– The VA currently will not pay for the surgeries necessary for one to transition to the opposite gender, will this hypothetical American single payer cover this cost, and how?
All are questions that Congress would have to address in any hypothetical piece of legislation. It is unfortunate that questions like these that were once easy to answer, might now be more difficult because of the social concerns that dominate the current political parties. This will lead to needless fights in justifying why one is more deserving of the other. Much like Eddie Rickenbacker is eligible for VHA benefits automatically, but an OIF/OEF Veteran must justify why he or she is deserving. Such duplicity does not bode well for those arguing that healthcare is a right. Furthermore, shifting the costs to the system for the oldest, and therefore most likely the sickest patients to Medicare illustrates a practice for a medical system designed to control costs simply by determining who is eligible through at best, arbitrary criteria. At worst, it may be determined by politically insidious criteria.
Such a practice in a hypothetical single payer system designed to cover all citizens is hardly equitable.
In terms of funding, there is no way to determine how much this will truly cost. Simply scaling up VHA to the present population is only a rough estimate and does not account for demographics. Simply put, most VHA eligible beneficiaries are men, between the ages of 55-65. This demographic has very specific and more importantly predictable needs which easily control costs, but are hardly indicative of the entire American population. Coupled with the unknown costs shifted to Medicare/Medicaid, any quantification that will be presented is simply dishonest.
For the audience which this piece is intended however, the moral case is simple: In order to participate in such a medical system an individual will necessarily need to justify the labor from skilled professionals while simultaneously reimbursing those professionals through appropriation made possible only by other individuals coerced into doing so. This is immoral as the previous sentence is a bunch of words more concisely described as theft. In the case of Veterans, at the very least they can point to a record where this appropriation was earned; the merits of which are understandably debatable for some and for others unjustified.
Eligibility for existing within a politically determined border, what kind of earned merit is that?
References
1) Longman, Phillip. Best Care Anywhere. Polipoint Press, February 2007. Pages 102-106.
2) Guina, Ryan. Funny Math–VA Disability Ratings. When 30+20 Doesn’t Always Equal 50. http://themilitarywallet.com/va-math-combined-disability-ratings/. 06/19/2017.
3) Zoroya, Greg. Shutdown holding up military, VA benefits.
https://www.usatoday.com/story/nation/2013/10/08/shutdown-casualties-combat-benefits -unpaid-pentagon/2941809/ 06/19/2017.
4) Dinan, Stephen. Veterans caught triple-dipping on benefits.
http://www.washingtontimes.com/news/2014/oct/30/veterans-caught-triple-dipping-on-benefits/ 06/19/2017.
5) Wasserman, Jeffery et al. Understanding Potential Changes to the Veterans Equitable Resource Allocation (VERA) System. http://www.rand.org/pubs/monographs/MG163.html.
6) Office of Inspector General. Report of Audit Congressional Concerns over Veterans Health Administration’s Budget Execution. https://www.va.gov/oig/52/reports/2006/VAOIG-06-01414-160.pdf.

 Get this man a presidency: Justin Amash
Get this man a presidency: Justin Amash 

 The Great Red Hope
The Great Red Hope
 The key to delivery in the VA is through the Primacy Care Provider (PCP). There is one doctor (MD), or nurse practitioner (NP) that is charged with providing the basis to all services to an individual Veteran. The team also has a small cadre of Registered Nurses (RN), Licensed Practical Nurses (LPN),
The key to delivery in the VA is through the Primacy Care Provider (PCP). There is one doctor (MD), or nurse practitioner (NP) that is charged with providing the basis to all services to an individual Veteran. The team also has a small cadre of Registered Nurses (RN), Licensed Practical Nurses (LPN), This means the PACT can focus on the types of issues older men typically face. Examples of such conditions include obesity, hypertension, diabetes or any condition that will worsen over time if a relationship with a physician is not maintained. If a condition worsens, the PCP will know about it and be in a good position to alter his or her plan of care. This proactive approach is often pointed out by advocates of single payer health care systems as a feature of these systems since most of the time healthcare in the United States is a reactive proposition. Reactive in the sense that most people will simply wait until that bump gets bigger, or that knee becomes too unbearable to walk on, or it hurts too much to urinate in the morning before finally making an appointment to see a doctor.
This means the PACT can focus on the types of issues older men typically face. Examples of such conditions include obesity, hypertension, diabetes or any condition that will worsen over time if a relationship with a physician is not maintained. If a condition worsens, the PCP will know about it and be in a good position to alter his or her plan of care. This proactive approach is often pointed out by advocates of single payer health care systems as a feature of these systems since most of the time healthcare in the United States is a reactive proposition. Reactive in the sense that most people will simply wait until that bump gets bigger, or that knee becomes too unbearable to walk on, or it hurts too much to urinate in the morning before finally making an appointment to see a doctor.  The thing is, most major hospital systems and private practices do not worry too much about whether or not they are able to schedule patients in a timely manner. The reason being, they have many fixed costs that are baked into their operating budgets. Paying for the cost of operations requires treating patients. If they can’t get patients into beds, they go under–kind of like when airlines have no passengers. The private sector is also large enough at the moment that if a patient cannot be seen at one place, they can find another. In the grand scheme of things it is about as difficult to schedule an HVAC technician as it is to schedule an appointment with a private doctor—it just depends on where you live, and the local supply and demand for services.
The thing is, most major hospital systems and private practices do not worry too much about whether or not they are able to schedule patients in a timely manner. The reason being, they have many fixed costs that are baked into their operating budgets. Paying for the cost of operations requires treating patients. If they can’t get patients into beds, they go under–kind of like when airlines have no passengers. The private sector is also large enough at the moment that if a patient cannot be seen at one place, they can find another. In the grand scheme of things it is about as difficult to schedule an HVAC technician as it is to schedule an appointment with a private doctor—it just depends on where you live, and the local supply and demand for services.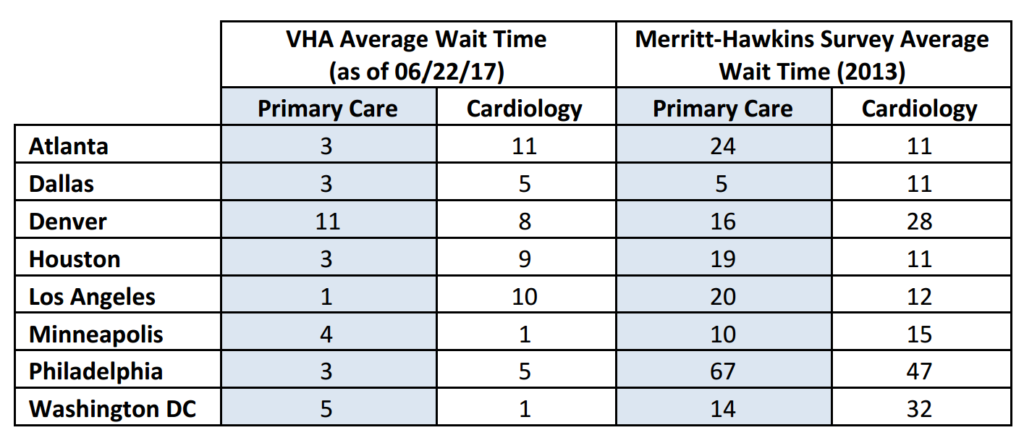
 AH! ➔ Appointment with PCP ➔ PCP Agrees and writes up a consult ➔Specialist receives consult and reviews ➔ Specialist accepts and schedules appointment ➔ Treatment ➔ Specialist documents treatment ➔ Specialist informs PCP of treatment ➔ Re-evaluation by PCP if needed.
AH! ➔ Appointment with PCP ➔ PCP Agrees and writes up a consult ➔Specialist receives consult and reviews ➔ Specialist accepts and schedules appointment ➔ Treatment ➔ Specialist documents treatment ➔ Specialist informs PCP of treatment ➔ Re-evaluation by PCP if needed. 
 If advocates of free markets, Federalism and personal responsibility are to define coherent arguments against such a system it is best they first understand what the future may look like. While the practical experience in Western Europe should provide enough ammunition, it is likely these systems will be used as arguments for single payer systems. It should however be noted, the experience in these countries are unlikely to be comparable to the United States, because these governments historically are more enthusiastic(?) in their approach to governance. Not to mention the centralized nature of the population and demographic homogeneity make it easier for these socialized systems to be implemented. An American example is needed–and fortunately is available for interpretation. It is this way freedom advocates will know, and knowing is half the battle.
If advocates of free markets, Federalism and personal responsibility are to define coherent arguments against such a system it is best they first understand what the future may look like. While the practical experience in Western Europe should provide enough ammunition, it is likely these systems will be used as arguments for single payer systems. It should however be noted, the experience in these countries are unlikely to be comparable to the United States, because these governments historically are more enthusiastic(?) in their approach to governance. Not to mention the centralized nature of the population and demographic homogeneity make it easier for these socialized systems to be implemented. An American example is needed–and fortunately is available for interpretation. It is this way freedom advocates will know, and knowing is half the battle. While Eddie Rickenbacker does not need to worry about paying for a colonoscopy, there are others with ailments such as Agent Orange or Gulf War Syndrome that were affiliated with wars that were determined by popular culture to be unpopular from a political standpoint, and were thus swept under the rug.
While Eddie Rickenbacker does not need to worry about paying for a colonoscopy, there are others with ailments such as Agent Orange or Gulf War Syndrome that were affiliated with wars that were determined by popular culture to be unpopular from a political standpoint, and were thus swept under the rug. For most sane individuals with the most rudimentary of education, 10+10+20=40, right?
For most sane individuals with the most rudimentary of education, 10+10+20=40, right? The bottom line is, the more service connected the Veteran is and the greater resources it would theoretically take to treat the Veteran individually, the more money the VAMC receives from Washington. This is not just for the big things like, a prosthetic or a cochlear implant that are SC, this also works for little things like flu shots and almost everything else Veterans use that is not SC. The dirty secret is, most services Veterans use at a VAMC are not SC, even if he or she is 100%. This funding system is called Veteran’s Equitable Resource Allocation (VERA).
The bottom line is, the more service connected the Veteran is and the greater resources it would theoretically take to treat the Veteran individually, the more money the VAMC receives from Washington. This is not just for the big things like, a prosthetic or a cochlear implant that are SC, this also works for little things like flu shots and almost everything else Veterans use that is not SC. The dirty secret is, most services Veterans use at a VAMC are not SC, even if he or she is 100%. This funding system is called Veteran’s Equitable Resource Allocation (VERA).